INTRODUCTION
Sugar-sweetened beverages (SSBs), defined as beverages containing added caloric sweeteners, have emerged as a major global public health concern driven by urbanization, large-scale manufacturing, and aggressive marketing by multinational beverage industries(1). Global consumption has risen steadily since the 1990s, particularly among children, adolescents, and young adults, with the fastest growth observed in low- and middle-income countries (LMICs) (2). High SSB intake substantially contributes to the global burden of non-communicable diseases (NCDs), accounting for millions of cases of type 2 diabetes and cardiovascular diseases and a rising number of premature deaths annually (3,4,5). Worldwide sugar availability exceeds World Health Organization (WHO) recommendations, and India reflects this trend with increasing intake across urban and rural populations, rising obesity, and metabolic risk, prompting policy responses such as taxation and food labelling reforms (4,5,6).

Epidemiology and Demographics of SSB Consumption (Global & India Focus)
The burden of SSB consumption has shifted from high-income countries to LMICs, particularly in the Global South, where it is now a major driver of NCDs(1). While fiscal policies have slowed intake in some high-income settings, multinational beverage companies continue to expand aggressively into emerging markets. Globally, the prevalence of high SSB intake among young adults (15–39 years) increased from 6.6% in 1990 to over 11.1% in 20212. SSB consumption contributes to approximately 2.2 million new cases of type 2 diabetes and 1.2 million cardiovascular disease cases annually, with attributable deaths increasing from about 150,000 in 1990 to over 240,000 in the 2020s (3,4,5). FAOSTAT data indicate that global per-capita sugar availability (~65 g/day) far exceeds the WHO-recommended limit of <25 g/day (4,5). India exemplifies this rapid nutrition transition. NFHS-5 and allied national data show increasing displacement of traditional diets by ultra-processed foods and SSBs(6). About 22.4% of men and 0.7% of women aged 15–49 report alcohol drink consumption, with higher intake among adolescents, males, and urban populations, though rural consumption is rising through affordable small-pack sales(7,8). Overweight and obesity among Indian men increased by 146% between NFHS-3 and NFHS-5, while retail sales of ultra-processed foods and beverages grew at a CAGR of 13.7% between 2011 and 2021, reaching USD 37.9 billion(9). Average sugar intake in India is estimated at ~25 kg/person/year, far exceeding WHO recommendations, with higher income and literacy initially correlating with increased consumption (10,11).
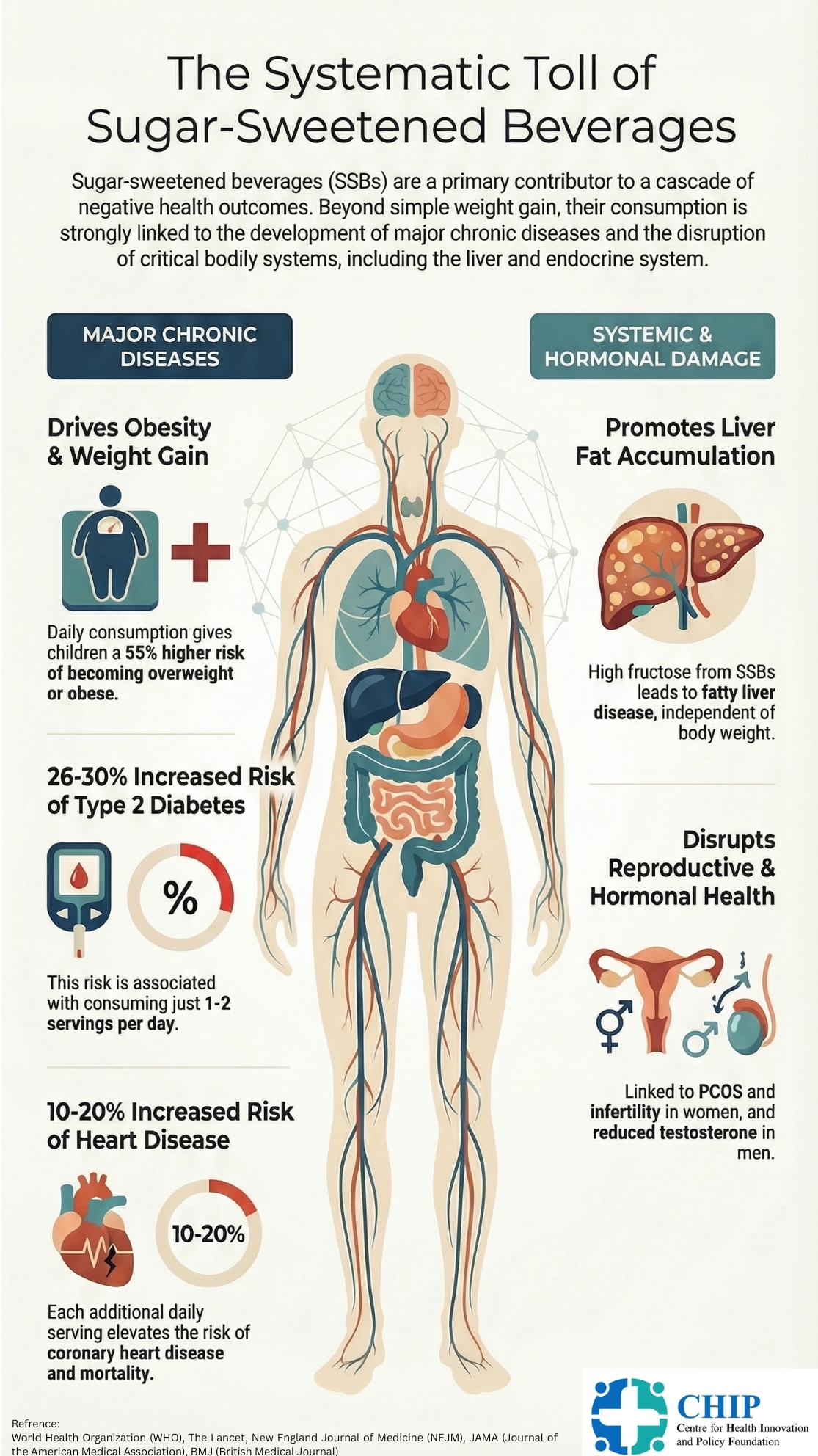
Health Impacts of Sugar-Sweetened Beverages
1. Excess Energy Intake, Weight Gain, and Obesity
SSBs provide large amounts of rapidly absorbable sugars with minimal satiety, leading to excess energy intake and weight gain. Each additional daily serving is associated with approximately 0.45 kg greater weight gain over four years in adults, while children consuming ≥1 SSB/day have a 55% higher risk of overweight or obesity (12). WHO concludes that reducing SSB intake lowers population-level obesity risk (13).
2. Type 2 Diabetes Mellitus
Habitual SSB consumption is strongly associated with type 2 diabetes, even after adjustment for body mass index, suggesting mechanisms beyond adiposity. Intake of 1–2 servings/day increases diabetes risk by 26–30%, with a substantial proportion of global diabetes incidence attributable to SSBs (14,15).
3. Cardiovascular Disease
SSB intake is linked to coronary heart disease, stroke, and cardiometabolic mortality through mechanisms including insulin resistance, dyslipidaemia, endothelial dysfunction, and inflammation. Each additional daily serving increases coronary heart disease risk by 10–20% and is associated with higher cardiovascular and all-cause mortality(15,16).
4. Liver Disease and MAFLD
SSBs are a major source of dietary fructose, promoting hepatic fat accumulation, insulin resistance, and inflammation (17,18). In postmenopausal women, daily sugar-sweetened beverage consumption (≥1 serving/day) was associated with an approximately 85% higher risk of hepatocellular carcinoma and a 68% higher risk of chronic liver disease mortality, compared with low intake (19). Fructose-induced hepatic fat accumulation occurs independent of body weight and contributes to metabolic dysfunction–associated fatty liver disease (MAFLD), which is closely linked to cardiovascular mortality (18,20,21,22).
5. Sexual Hormones and Reproductive Health
SSB-induced insulin resistance and adiposity disrupt endocrine homeostasis. Chronic hyperinsulinemia suppresses hepatic sex hormone–binding globulin (SHBG), increasing free sex hormone levels and cardiometabolic risk(20). In women, high SSB intake contributes to hyperandrogenism, polycystic ovary syndrome (PCOS), menstrual irregularities, and infertility, making sugar reduction central to PCOS management(23). In men, excess sugar intake is associated with visceral adiposity, reduced testosterone, infertility, sarcopenia, and adverse cardiometabolic outcomes (24).

Taxation on Sugar-Sweetened Beverages in India
SSBs classified under HSN code 2202 are subject to taxation under India’s GST framework (25). Following the 56th GST Council meeting in September 2025, SSBs were placed under a “sin tax” category, with a uniform 40% GST rate applied to aerated and sugar-sweetened beverages (26-29). This replaced the earlier structure of 28% GST plus a 12% compensation cess, maintaining an effective deterrent rate while simplifying taxation(25,27). The policy aligns with WHO recommendations advocating 20–50% taxation to reduce consumption and generate revenue for health programs (30,31). Health Burden and Economic Rationale Globally, over 50 countries have implemented SSB taxes, achieving average consumption reductions of 10–15% (31) Modeling studies suggest that increasing India’s tax to 50% and earmarking revenues for health and nutrition programs could further enhance public health impact (30–32). From a health economics perspective, SSB taxation functions as a Pigovian tax, correcting externalities linked to healthcare costs and productivity losses from obesity and diabetes (30,33). India’s current 40% GST is projected to reduce consumption by 10–20%, avert future NCD cases, and generate fiscal space for public health investment (33,34,35).

Labelling of SSBs
Food labelling in India is regulated by the Food Safety and Standards Authority of India (FSSAI) under the Food Safety and Standards Act, 2006(36). Mandatory labelling includes nutritional information, ingredient lists, and declaration of added sugars, though no specific warning labels for high sugar content are currently required. Evidence shows that health warnings significantly reduce SSB purchase intentions and consumption, particularly among children (37,38). While several jurisdictions in the USA have proposed warning labels, only San Francisco has implemented them(39).
In September 2022, FSSAI issued draft amendments proposing Front-of-Pack Nutrition Labelling (FOPNL), identification of High Fat, Sugar, and Salt (HFSS) foods, disclosure of key ingredient percentages, dietary fiber content, and introduction of the Indian Nutrition Rating (INR) system(40). The INR assigns star ratings from 0 (least healthy) to 5 (healthiest), enabling consumers to make informed choices.
CONCLUSION
Regular consumption of sugar-sweetened beverages is a major contributor to India’s rising burden of obesity, type 2 diabetes, cardiovascular disease, MAFLD, and oral health disorders. As SSBs become increasingly normalized and aspirational among youth and rural populations, comprehensive policy action is essential. While the recent 40% GST “sin tax” represents progress, strengthening taxation, mandating Front-of-Pack labelling through the INR system, introducing health warning labels, and implementing sustained public awareness campaigns are critical to reducing consumption, improving population health, and mitigating long-term economic and healthcare burdens.
References:
1) Popkin BM. Nutrition transition and the global diabetes epidemic. CurrDiab Rep 2015;15:64.
2) Ge C, Xiong J, Zhu R, Hong Z, He Y. Global burden of high sugar-sweetened beverage consumption among young adults. DiabetolMetabSyndr 2025;17:259.
3) Lara-Castor L, O’Hearn M, Cudhea F, et al. Burdens of type 2 diabetes and cardiovascular disease attributable to sugar-sweetened beverages in 184 countries. Nat Med 2025;31:552–64.
4) Lara-Castor L, Micha R, Cudhea F, et al. Intake of sugar-sweetened beverages among children and adolescents in 185 countries between 1990 and 2018: A population-based study. BMJ 2024;386:e079234.
5) Global Burden of Disease Collaborators. Mortality and DALY trends in high sugar-sweetened beverage intake cohorts, 1990–2021. Seattle: Institute for Health Metrics and Evaluation; 2024.
6) UNICEF India. Feeding profit: How food environments are failing children. New Delhi: UNICEF; 2025.
7) International Institute for Population Sciences. National Family Health Survey (NFHS-5), 2019–21: India. Mumbai: IIPS; 2021.
8) RajyaSabha Secretariat. Excessive sugar and sodium content in cold drinks. New Delhi: Ministry of Health and Family Welfare, Government of India; 2025.
9) UNICEF India. Overweight and obesity rising across all ages – from youngest children to adults. New Delhi: UNICEF; 2024.
10) Varghese B, Panicker R, Mukhopadhyay D, et al. Estimating the potential impact of a health tax on the demand for unhealthy food and beverages and on tax revenue in India. Health Policy Plan 2024;39:299–306.
11) Mathur MR, Nagrath D, Malhotra J, Mishra VK. Determinants of sugar-sweetened beverage consumption among Indian adults: Findings from NFHS-4. Indian J Community Med 2020;45:60–5.
12) Malik VS, Pan A, Willett WC, Hu FB. Sugar-sweetened beverages and weight gain in children and adults: A systematic review and meta-analysis. Am J ClinNutr 2013;98:1084–102.
13) World Health Organization. Guideline: Sugars intake for adults and children. Geneva: WHO; 2015.
14) Imamura F, O’Connor L, Ye Z, et al. Consumption of sugar-sweetened beverages and incidence of type 2 diabetes. BMJ 2015;351:h3576.
15) Malik VS, Hu FB. Sugar-sweetened beverages and cardiometabolic health. Lancet 2019;393:1970–8.
16) Fung TT, Malik V, Rexrode KM, Manson JE, Willett WC, Hu FB. Sweetened beverage consumption and risk of coronary heart disease in women. Am J ClinNutr 2009;89:1037–42.
17) Stanhope KL. Sugar consumption, metabolic disease and obesity: The state of the controversy. Physiol Rev 2016;96:1–54.
18) Tappy L, Lê KA. Metabolic effects of fructose and the worldwide increase in obesity. Physiol Rev 2010;90:23–46.
19) Debras C, Chazelas E, Srour B, et al. Sugar-sweetened and artificially sweetened beverages and risk of liver cancer and chronic liver disease mortality. JAMA 2023;330:537–46.
20) Ding EL, Song Y, Malik VS, Liu S. Sex differences of endogenous sex hormones and risk of type 2 diabetes. N Engl J Med 2009;361:1152–63.
21) Teede HJ, Misso ML, Costello MF, et al. International evidence-based guideline for the assessment and management of polycystic ovary syndrome. Hum Reprod 2018;33:1602–18.
22) Stanhope KL, Schwarz JM, Keim NL, et al. Consuming fructose-sweetened beverages increases visceral adiposity and lipids. J Clin Invest 2009;119:1322–34.
23) Eslam M, Newsome PN, Sarin SK, et al. A new definition for metabolic dysfunction–associated fatty liver disease. Lancet GastroenterolHepatol 2020;5:17–30.
24) Grossmann M. Low testosterone in men with type 2 diabetes: Significance and treatment. Lancet Diabetes Endocrinol 2014;2:287–98.
25) GST Council slaps highest tax rate on aerated and other sugar-based drinks. Economic Times. September 3, 2025.
26) Global Alliance for Improved Nutrition. Can the 2025 GST reforms make Indians eat healthier diets? New Delhi; 2025.
27) TwoTax. New GST rates for food and beverages from 22 September 2025. 2025.
28) ClearTax. GST on cold drinks: Tax rates, HSN code and impacts. 2025.
29) India Today. India’s new GST reform puts cola and energy drinks in the sin tax bracket. September 4, 2025.
30) World Bank. A diagnostic of the health taxes landscape in India. Washington DC: World Bank; 2025.
31) Khodadadpoor S, et al. Impacts of sugar-sweetened beverage taxes on health and economic outcomes: An umbrella review. Health Scope 2024.
32) Cabrera Escobar MA, et al. Taxation of tobacco, alcohol, and sugar-sweetened beverages. BMJ Glob Health 2023;8(Suppl 8):e011866.
33) Health and economic effects of increased taxation on tobacco, alcohol, and sugary drinks in India: A modelling study. Lancet Public Health 2025.
34)Basu S, Vellakkal S, Agrawal S, et al. Averting obesity and type 2 diabetes in India through sugar-sweetened beverage taxation. PLoS Med 2014;11:e1001582.
35) Sharma R, et al. Modelling and empirical evidence of the impact of implementation of sugar-sweetened beverage taxes. 2024.
36) Food Safety and Standards Authority of India. Food Safety and Standards Act, 2006. New Delhi: FSSAI.
37) Grummon AH, Hall MG. Sugary drink warnings: A meta-analysis of experimental studies. PLoS Med 2020;17:e1003120.
38) Hall MG, Grummon AH, Higgins ICA, et al. Impact of pictorial health warnings on purchases of sugary drinks for children. PLoS Med 2022;19:e1003885.
39) Cities and states consider warning labels on sugary drinks. STAT. 2016.
40) Food Safety and Standards Authority of India. Front-of-pack nutrition labelling draft regulations. New Delhi: FSSAI; 2022